What Is a Goiter?
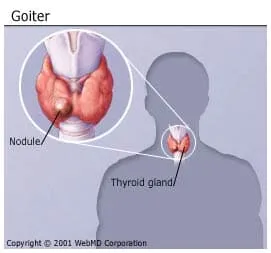
A goiter is an enlargement of your thyroid gland. That's the gland at the front of your neck just below your Adam's apple.
It may be a temporary problem that will get better without treatment. Or it can be a symptom of another, possibly serious, thyroid condition that requires medical attention.
Types of Goiters
Since many things can make your thyroid swell, there are lots of types of goiters. A few of them are:
Simple goiters, which happen when your thyroid gland doesn't make enough hormones. The thyroid grows larger to make up for this.
Endemic goiters. Sometimes called colloid goiters, these are caused by a lack of iodine in your diet. Your thyroid uses iodine to make its hormones. Few people get this kind of goiter in countries where iodine is added to table salt, like the United States.
Sporadic or nontoxic goiters, which usually have no known cause. Certain drugs and medical conditions can trigger them.
Multinodular goiters, which happen when lumps called nodules grow in your thyroid.
A goiter is described as "toxic" when it's linked to hyperthyroidism. That means your thyroid makes too much thyroid hormone. A "nontoxic" goiter doesn't cause ether hyperthyroidism or hypothyroidism (not enough thyroid hormone).
Goiter Symptoms
The symptoms of a goiter include swelling at the front base of the neck, ranging from a small lump or multiple nodules to a general enlargement on one or both sides of your neck.
You may also have:
- A hoarse voice
- Tightness in your throat
- Dizziness when you raise your arms
- Swollen neck veins
- Coughing
- Trouble breathing or swallowing
If you have a toxic goiter with hyperthyroidism, you might have:
- Sweating
- Diarrhea
- Nausea
- A fast pulse or heartbeat
- Shakiness or hand tremors
- Weight loss despite an increased appetite
- High blood pressure
- An overheated feeling
- Nervousness
- Muscle weakness
If you have hypothyroidism, you could notice:
- Dry skin
- Tiredness
- Weight gain
- Constipation
- An irregular period
- Slowed physical and mental functions
- Depression
- A lower heart rate
- A cold feeling
- Tingling or numbness in your hands
Goiter Causes and Risk Factors
Goiters don't represent any one disease. They can form quickly or very slowly over years.
Before iodized salt was introduced in 1920, iodine deficiency was the main cause of goiters in the U.S. It still is worldwide.
In the U.S., the main causes of goiters are autoimmune disorders (including Graves' disease or Hashimoto's disease) and multinodular goiter.
Inflammation of the thyroid, called thyroiditis, can also cause a goiter. You can get this after getting sick from a virus or after giving birth.
Risk factors for goiters include:
- Age. You're at higher risk if you're over 40.
- Gender. Women are more likely to have goiters and thyroid disorders overall.
- Pregnancy or menopause, both of which are linked to thyroid issues
- History of autoimmune disease
- Some medications, including lithium (used for mood disorders) and amiodarone (for irregular heartbeat)
- Exposure to radiation, such as cancer treatments
- Living in an area where iodine deficiencies are common
Goiter Diagnosis
Often, your doctor will diagnose your goiter simply by examining your neck. You may then have tests to find out what caused it and how it affects you. They include:
- An ultrasound to see how large your thyroid is and whether you have nodules
- Blood tests to measure your thyroid hormone levels and see whether you have the antibodies that some goiters cause. Antibodies are proteins your body makes to fight infection.
- A biopsy, where your doctor uses a thin needle to take a sample of tissue or fluid for testing. This is used to rule out cancer.
- A thyroid scan, in which your doctor injects a little radioactive material to create an image of your thyroid on a computer screen. This shows your doctor the size of your thyroid and how well it's working.
- A CT scan orMRI if your goiter is large or has spread to your chest
Goiter Treatment
A goiter may not need treatment, especially if it is small and thyroid hormone levels are normal. But if your thyroid hormone levels are too high or too low, you will need treatment.
Treatment involves getting the thyroid hormone levels back to normal. Depending on what caused your goiter and how serious it is, your doctor can treat it with:
- Medication. If you have hypothyroidism, your doctor may prescribe a thyroid hormone replacement medication. When the medication takes effect, the thyroid may begin to return to its normal size. But a large nodular goiter with a lot of internal scar tissue will not shrink with treatment. For goiters caused by inflammation, you might take aspirin or corticosteroids.
- Surgery. If the goiter is uncomfortable, causes overproduction of thyroid hormone unresponsive to medications, is large enough that it causes symptoms because of its size, or becomes cancerous, the entire thyroid gland may have to be surgically removed. Or they might take out only part of it. Afterward, you may need to take thyroid hormone medicine for the rest of your life.
- Radioactive iodine. You take this in a pill to treat an overactive thyroid. It kills cells to shrink the thyroid. After this treatment, you'll probably need to take hormone drugs from then on.
If you have a goiter, your doctor may want to check it on a periodic basis with ultrasound to be sure that it isn’t growing larger or developing suspicious looking nodules that might call for a fine-needle biopsy.
Call Your Doctor About a Goiter If:
You should call the doctor if you experience any of the above symptoms with a goiter because you may have hyperthyroidism or hypothyroidism that needs treatment. Goiters are slow-growing, but if you have a large goiter and notice shortness of breath or voice changes, you should call the doctor. The goiter may be pressing on your jugular vein, windpipe, esophagus, or the nerve that runs to your larynx. The growth requires treatment and may need to be surgically removed.

