What Are Stomach Ulcers?
Stomach ulcers, also known as peptic ulcers, are open sores in the lining of your stomach or the upper part of your small intestine. The ulcer forms when stomach acid eats away at the mucus that protects the lining of your digestive tract.
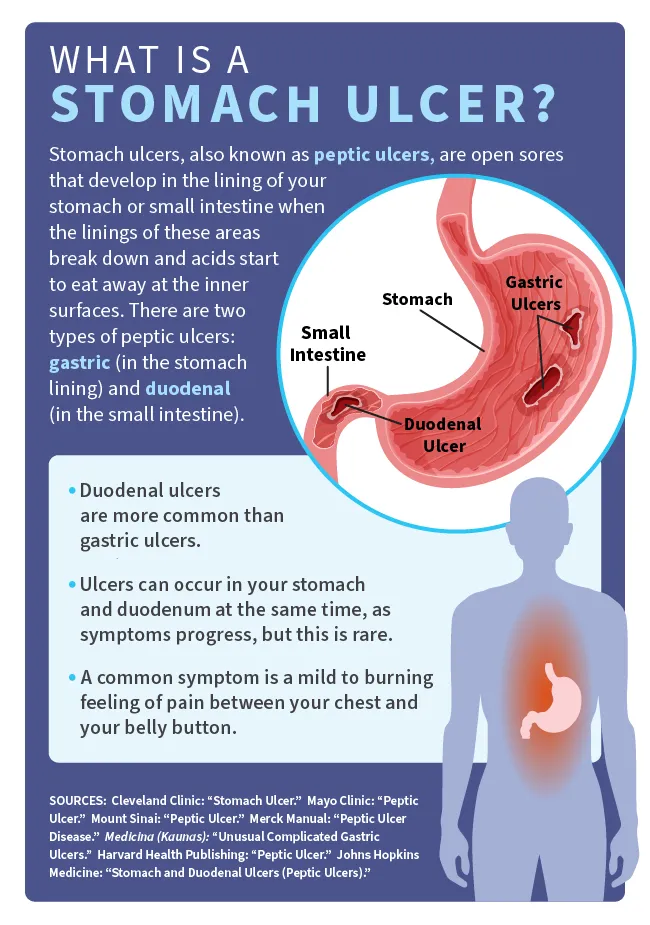
Types of peptic ulcers
- Gastric ulcer: It occurs when a sore forms in the lining of your stomach.
- Duodenal ulcer: This happens when a sore develops in the upper part of your intestine.
- Esophageal ulcer: This is when a sore forms in the lining of your esophagus, which is the tube that carries food and liquid from your throat to your stomach.
About 1 in 10 Americans experience the burning, gnawing abdominal pain of a peptic ulcer at some point in life. Duodenal ulcers are more common than stomach ulcers. Esophageal ulcers are more rare and are often a result of certain medications, such as some antibiotics and anti-inflammatories, or alcohol abuse.
Causes of Stomach Ulcers
Until the mid-1980s, the conventional wisdom was that ulcers form as a result of stress, being prone to excessive stomach acid secretion because of genetics, and poor lifestyle habits (including overindulging in rich and fatty foods, alcohol, caffeine, and tobacco). It was believed that such factors could lead to a buildup of stomach acids that could erode the protective lining of the stomach, duodenum, or esophagus.
While too much stomach acid secretion certainly plays a role in the development of ulcers, a relatively recent theory holds that bacterial infection is the primary cause of peptic ulcers. Research since the mid-1980s has shown that the bacterium Helicobacter pylori (H. pylori) is present in more than 90% of duodenal ulcers and about 80% of stomach ulcers. However, more recent figures indicate those percentages are declining.
Most people infected with H. pylori do not get ulcers. But in others, it can raise the amount of acid, break down the protective mucus layer, and irritate the digestive tract. Experts aren’t sure how an H. pylori infection spreads. They think it may pass from person to person through close contact, such as kissing. You may also get it from unclean food and water.
Other factors also seem to contribute to ulcer formation, especially in someone with an H. pylori infection, including:
- Overuse of over-the-counter painkillers (such as aspirin, ibuprofen, and naproxen). If you’ve been taking aspirin often and for a long time, you’re more likely to get a peptic ulcer. The same is true for other nonsteroidal anti-inflammatory drugs (NSAIDs). They include ibuprofen and naproxen. NSAIDs block your body from making a chemical that helps protect the inner walls of your stomach and small intestine from stomach acid. Other types of pain meds, such as acetaminophen, won’t lead to peptic ulcers.
- Heavy alcohol use
- Psychological stress
- Smoking
Your risk for peptic ulcers also increases if you:
- Use steroids and have high calcium levels. If you use steroids often and have high levels of calcium in your blood, known as hypercalcemia, you can be more prone to ulcers.
- Are older. Studies show that stomach ulcers are more likely to develop in older people. This may be because arthritis is prevalent in older people, and easing arthritis pain can mean taking daily doses of aspirin or ibuprofen. Also, with advancing age, the pylorus (the valve between the stomach and duodenum) relaxes and allows extra bile (a compound produced in the liver to aid in digestion) to seep up into the stomach and erode the stomach lining.
- Have type A blood. For an unknown reason, people with type A blood are more likely to develop cancerous stomach ulcers.
- Have type O blood. Duodenal ulcers tend to appear in people with type O blood, possibly because they do not produce the substance on the surface of blood cells that may protect the lining of the duodenum.
- Have Zollinger-Ellison syndrome. If you have Zollinger-Ellison syndrome, which is a rare condition where tumors in your pancreas or duodenum (called gastrinomas) cause your stomach to make too much acid, you are at a greater risk of developing peptic ulcers.
Stomach Ulcer Symptoms
You’ll most likely feel a burning pain or discomfort between your belly button and breastbone. You might especially notice it on an empty stomach, such as between meals or at night. The pain may stop for a little while if you take an antacid, but it may return. The pain can last a few minutes or a few hours and may come and go for many days or weeks.
Other symptoms may include:
- Feeling easily full
- Not wanting to eat because of pain
- Heartburn
- Acid reflux
- Chest pain
- Fatigue
- Bloated feeling
- Burping
- Lack of appetite or weight loss
- Nausea
- Bloody or dark poop
- Vomiting that might contain blood or look like coffee grounds
- Anemia
- Pain that may improve when you eat, drink, or take antacids
Small ulcers may not cause any symptoms. But if you notice any of these signs, talk to your doctor.
How Are Stomach Ulcers Diagnosed?
If your doctor thinks you might have a peptic ulcer, they’ll probably start with a physical exam and some tests:
- They’ll feel your belly and ask if you’ve had things such as tenderness, pain, or bloating. They might use a stethoscope to listen to any sounds your stomach is making.
- The next step will be tests to look for signs of the H. pylori bacteria. Your doctor may take samples of your blood, stool, or breath for these.
- In some cases, especially if you’re older and your symptoms include things such as weight loss or loss of appetite, they might use a long, flexible tube called an endoscope to look down your throat and into your stomach for signs of an ulcer (you’ll be given medicine to make you sleepy). An endoscope can also take a small sample of tissue from an ulcer that can be tested in a laboratory.
- They might ask you to drink a milky liquid called barium before they take X-rays of your stomach. This drink coats your digestive system and makes problems such as ulcers show up more clearly.
Stomach Ulcer Treatment
If you have a peptic ulcer, your doctor will recommend a treatment plan based on what’s causing it.
The most common remedy is a combination of antibiotic drugs to kill the H. pylori bacteria and medications to get rid of acid in your stomach. These typically include proton pump inhibitors (PPIs), such as Aciphex or Nexium, and antibiotics. You’ll take PPIs for several weeks. There are other treatment options.
- If your ulcer is caused by over-the-counter painkillers, you’ll need to quit taking them.
- Your doctor may give you a drug called a cytoprotective agent, which coats ulcers to protect them from stomach acid.
- Your health care provider may also give you antacids to fight stomach acid or prescribe medicine to lessen the acid your body makes.
- Histamine receptor blockers, also known as H2 blockers, reduce the amount of acid produced in the stomach.
- Probiotics might help slow the growth of H. pylori.
- Bismuth supplements can also slow the growth of H. pylori.
Also, lifestyle changes can serve as a treatment for stomach ulcers. You might need to:
- Quit smoking.
- Drink less alcohol or caffeine.
- Stay away from foods that make your symptoms worse.
If your ulcers don’t improve with medication or lifestyle changes, sometimes surgery is necessary. Depending on your specific case, your doctor might recommend:
- Gastrectomy: It removes part of your stomach.
- Vagotomy: It cuts the vagus nerve, which causes you to make less acid.
- Antrectomy: It removes the lower part of the stomach, which produces a hormone that tells the body to make digestive juices.
- Pyloroplasty: It makes the opening to the duodenum and small intestine bigger. This helps food pass out of your stomach faster.
- Laparoscopic surgery: In this, the doctor uses a small tube with a camera to look for problems with your esophagus, stomach, and small intestine. Or, the doctor may operate using a very small opening.
After treatment, your doctor may want to keep a close eye on you, depending on the size and location of your ulcer, how well the treatment worked, and if you had any other problems.
Home Remedies for Stomach Ulcers
There are no home remedies for stomach ulcers, but certain foods and supplements may help fight the H. pylori bacteria. These include cruciferous vegetables (such as broccoli and cauliflower), leafy greens, fermented foods (such as sauerkraut and yogurt), apples, berries, olive oil, honey, probiotics supplements, vitamin C, and glutamine. If you have ulcers, avoiding spicy and acidic foods as well as cigarettes, caffeine, and alcohol may help your symptoms.
Stomach Ulcer Complications
Some ulcers heal on their own; however, if your ulcer goes untreated or you have recurrent ulcers, you may develop complications such as:
- Bleeding from the ulcer site that can become life-threatening
- Penetration, which happens when the ulcer goes through the wall of your digestive tract into another organ, such as the pancreas
- Perforation, which occurs when the ulcer creates a hole in the wall of your digestive tract
- Obstruction (blockage) in your digestive tract, which happens because of swelling of inflamed tissues
- A hole in your stomach, which may need to be fixed with surgery
- Stomach cancer, specifically non-cardia gastric cancer
Ulcers can also erode the blood vessel wall in your stomach or small intestine, and eat a hole through the lining, leading to infection. Or they can cause swelling, which may block food from moving from your stomach into your small intestine.
Stomach Ulcer Prevention
While stress and spicy foods can make symptoms of a peptic ulcer worse, they don’t seem to make you more likely to have one. But a few other things can raise your chances.
You're more likely to get an ulcer while taking NSAIDs if you:
- Are over age 65
- Are infected with H. pylori bacteria
- Take more than one NSAID at a time
- Have had a peptic ulcer in the past
Also take a steroid drug or selective serotonin reuptake inhibitor (SSRI)
Be careful when you take pain relievers such as aspirin, ibuprofen, and naproxen sodium. Some people who have arthritis or other conditions that cause chronic pain take NSAIDs for weeks or months at a time to ease pain and swelling. These medicines can affect the mucus that protects your stomach against acid and make you more likely to have peptic ulcers.
To lower your chances for peptic ulcers while you take NSAIDs:
- Use the lowest possible dose to control your symptoms, and stop taking them as soon as you no longer need them. Also, talk to your doctor about using a different pain reliever such as acetaminophen.
- Take your medicine with food.
Don't drink alcohol while you’re taking these medicines.
While you're on NSAIDs, you can take medicine to lower the amount of acid your stomach makes. Drugs that can do that include:
- Proton pump inhibitors (PPIs) such as esomeprazole (Nexium), omeprazole (Prilosec OTC), and pantoprazole (Protonix)
- H2 blockers such as cimetidine (Tagamet), famotidine (Pepcid), and nizatidine
You can also take the drug misoprostol (Cytotec) to boost the amount of protective mucus your stomach makes. But that can cause side effects including diarrhea and stomach cramps.
A few changes to your lifestyle can help reduce the risk of complications. Some include:
Don’t smoke, and limit alcohol. These two habits make you more likely to get peptic ulcers. Both thin the mucus lining that protects your stomach from acid, leading to more acid. Ask your doctor to recommend a program to help you quit smoking. And talk with them about how much alcohol is safe for you to drink.
Manage stress. Stress can make the symptoms of a peptic ulcer worse. Figure out what’s causing issues for you and see how you can deal with it better. For example, getting enough sleep can help with that. It also can boost your immune system.
Consider probiotics. Millions of bacteria normally live in your gut. Some, like H. pylori, cause disease. Others are good for you because they help crowd out harmful bacteria. These helpful bacteria are called probiotics.
They’re still being studied, but researchers think they may help with peptic ulcers. You can find them in foods such as:
- Dairy products that have live cultures, such as yogurt, kefir, and aged cheeses
- Sauerkraut
- Kimchi
- Miso
- Tempeh
Prevent H. pylori infection. About two-thirds of people around the world have this type of infection, but most don’t get ulcers because of it. Doctors don’t know how you can avoid H. pylori, but they think it spreads from person to person or through food or water.
You can also do some things to make an H. pylori infection less likely:
- Wash your hands often during the day with warm water and soap so you don't catch or spread H. pylori bacteria. Clean your hands before you eat and after you go to the bathroom. If you don't have soap and water close by, use an alcohol-based hand sanitizer.
- Cook meat and other foods all the way through.
- Only drink water that you know is clean.
Takeaways
Ulcers are very common, and early treatment with medications and lifestyle changes can heal them. Talk with your doctor if you have symptoms of an ulcer. These include heartburn, acid reflux, feeling full even when you don’t eat much, and having pain that goes away when you take antacids. Lifestyle changes can help when you have an ulcer. Quit smoking, drink less caffeine and alcohol, and avoid foods that make your symptoms worse.
Stomach Ulcer FAQs
What are the symptoms of peptic ulcer? Pain that may or may not improve when you eat, drink, or take antacids, feeling easily full, acid reflux, heartburn, anemia (symptoms can include tiredness, shortness of breath, or paler skin), chest pain, fatigue, and vomit that contains blood or looks like coffee grounds.
How serious is a peptic ulcer? Ulcers can lead to serious complications. If you suspect an ulcer, see your doctor.
Do peptic ulcers ever go away? Sometimes, ulcers can go away on their own, but it can take a long time and cause you pain. They often recur. See your doctor if you suspect an ulcer.
How do they fix a peptic ulcer? A peptic ulcer can be treated with medication, lifestyle changes, and surgery.

